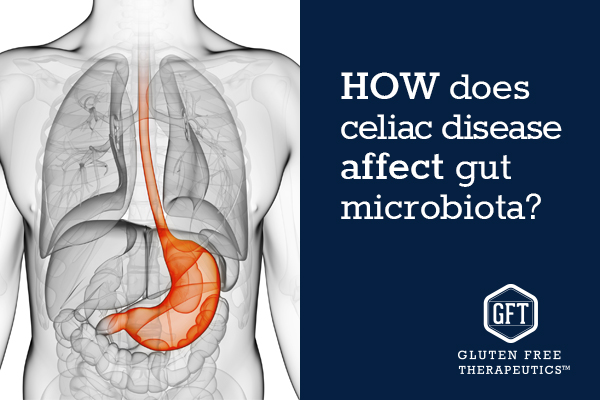
Celiac Patients and Gut Microbiota
By Alex Reis PhD, GFT science writer
From the moment we’re born, every nook and cranny in our body is invaded by an army of invisible microbes intent on staying with us for the rest of our lives. Of all possible locations, the gastrointestinal tract is undoubtedly the most heavily populated organ, with an incredible 100 trillion bacteria from over 1,000 different species and collectively carrying 150 times as many genes as those in our genome. These “partners” we carry around with us can be either friend or foe, developing a fine balance which can be the difference between health and disease.
Since the Human Microbiome Project launched in 2008, the massive impact these tiny organisms can have in our health is slowly being unveiled. From the expected irritable bowel syndrome (IBS) to the rather surprising cardiovascular conditions and depression, the list of conditions that can be affected by an unbalanced microbiota keeps on growing. Celiac disease is one of those conditions.
How does celiac disease affect gut microbiota?
Like a finger print, each person has its own unique bacterial profile. There may be space for individuality, but most healthy individuals eating a balanced diet end up developing a rather friendly group of microbes, mostly dominated by gram-positive bacteria. These bacteria are very good at keeping invading pathogens at large and inhibiting food antigens, including from gluten.
This property would be extraordinarily useful for celiac patients. However, their gut microbiota may start on a “positive” note, but it’s gradually replaced by harmful gram-negative bacteria instead. As the balance starts to shift, these inflammation-causing bacteria take advantage of gram-positive’s weakened status and further aggravate the patient’s gluten intolerance.
The most important loss in gram-positive bacteria is seen in lactobacillus, bifidobacteria and some clostridium groups. Some of these, for example, are butyrate producers, an important energy source for intestinal cells, while others have essential anti-inflammatory properties.
As a result, the gut microbiota of celiac patients becomes dominated by the gram-negative Bacteroides-Prevotella group. Under normal circumstances, the gut is capable of keeping their inflammatory properties in check, but the system goes into overload as the numbers start to accumulate. Higher numbers of inflammatory-causing bacteria and a feeble immune response mean a constantly inflamed gut mucosa in celiac patients.
Can a gluten free diet solve the problem?
Currently, a gluten-free diet is the only available treatment for celiac patients. This diet alleviates many of the symptoms, but somewhat surprisingly, studies suggest it does not completely restore healthy microbiota profiles. It does restrict the presence of infection-causing bacteria, such as E. Coli, but there are some subtle changes caused by celiac disease that cannot be reverted.
It seems that it may be the diet itself preventing complete restoration of normal microbial patterns. Even in healthy patients subject to a gluten-free diet, the delicate balance between gram-positive and gram-negative is lost, with healthy bacteria quickly replaced by opportunistic pathogens. The long-term result may be weaker immune defences and chronic inflammation.
Interestingly, a diet that frequently leads to a lower intake of complex carbohydrates could explain these changes: normally these compounds reach the colon partially undigested and constitute an important energy source for friendly bacteria. Without this “food” supply, these bacteria lose their competitive advantage against any potential invaders.
This sets up a scenario where even a strict gluten free diet may leave celiac patients still susceptible to inflammation and infections, and potentially suffering rather unpleasant symptoms not to mention increased health risks. The answer may include better dietary counselling for celiac patients, including ways to promote a stable polysaccharide intake and appropriate diet supplementation.
This original article is made possible by Gluten Free Therapeutics. Our mission is to educate, inform, and provide the most effective nutritional products possible to allow those with celiac disease and serious gluten intolerances to heal their bodies. CeliVites complete line of superior gluten free supplements includes multivitamin/multimineral supplements, iron supplements, and calcium supplements for people living with celiac disease. All CeliVites products are designed to help you heal, restore and rebuild your body, because going gluten free isn’t enough!
REFERENCES
- De Palma G, Nadal I, Medina M, Donat E, Ribes-Koninckx C, Calabuig M, and Sanz Y. Intestinal dysbiosis and reduced immunoglobulin-coated bacteria associated with coeliac disease in children. BMC Microbiol. 2010; 10: 63.
- Di Cagno R, De Angelis M, De Pasquale I, Ndagijimana M, Vernocchi P, Ricciuti P, Gagliardi F, Laghi L, Crecchio C, Elisabetta Guerzoni M, Gobbetti M, and Francavilla R. Duodenal and faecal microbiota of celiac children: molecular, phenotype and metabolome characterization. BMC Microbiol. 2011; 11: 219.
- Francavilla R, Ercolini D, Piccolo M, Vannini L, Siragusa S, De Filippis F, De Pasquale L, Di Cagno R, Di Toma M, Gozzi G, Serrazanetti D, De Angelis M and Gobbettic M. Salivary Microbiota and Metabolome Associated with Celiac Disease. Appl Environ Microbiol. 2014; 80(11): 3416–3425.
- Golfetto L, de Senna F, Hermes J, Soares Beserra B, da Silva Franca F and Martinello F. Lower Bifidobacteria counts in adult patients with celiac disease on a gluten-free diet. Arq Gastroenterol. 2014; 51: 139-143
- Nadal I, Donat E, Ribes-Koninckx C, Calabuig M and Sanz Y. Imbalance in the composition of the duodenal microbiota of children with coeliac disease. J Med Microbiol. 2007; 56 (12):1669-1674
- Pozo-Rubio T, Olivares M, Nova E, De Palma G, R. Mujico J, Desamparados Ferrer M, Marcos A, and Sanz Y. Immune Development and Intestinal Microbiota in Celiac Disease. Clin Dev Immunol. 2012; 2012: 654143.
- Sánchez E, Donat E, Ribes-Koninckx C, Fernández-Murga ML and Sanz Y. Duodenal-Mucosal Bacteria Associated with Celiac Disease in Children. Appl Environ Microbiol. 2013; 79(18): 5472–5479.
- Sanz Y. Effects of a gluten-free diet on gut microbiota and immune function in healthy adult humans. Gut Microbes. 2010; 1(3): 135–137.
- Schippa S, Lebba V, Barbato M, Di Nardo G, Totino V, Proietti Checchi M, Longhi C, Maiella G, Cucchiara S, and Pia Conte M. A distinctive ‘microbial signature’ in celiac pediatric patients. BMC Microbiol. 2010; 10: 17
Comments ()












thank you for sharing
I’m a celiac patient struggling to find a dietician or nutritionist in CT that actually knows enough about celiac to help me with my diet. The other road block is, all the ones I’ve contacted so far tell me insurance won’t cover for celiac treatments, but they do for diabetes. What? Can you recommend where I may find help with my diet? Even if it’s far, perhaps skype would work.
Wendy, we cannot recommend a nutritionist for you. But we do have a resource for you that may help. The celiac disease foundation has a celiac practitioners resource directory that you may want to try. The link is http://celiac.org/celiac-disease/provider-directory/
They may be able to help you find a professional to help with your questions regarding the CD diet.
I will take note of the celiac practioners resource directory you mentioned above. My husband follows a GF diet I’m not sure if it is because in 1980 he had surgery to remove 10 % of his stomach due to ulcers and was left with 10% instead. So even though he follows a GF diet he seems to get body cramping after eating, exercise etc. He also has paraxamal dystonia, I think this is one of the most heartbreaking diseases because when his body twists and cramps it is very disabling. Many of the people we know with celiac also have body cramping. do you find a connection.
Wendy: If you get a letter written by your doctor explaining that the GF diet is medically necessary and very difficult to implement so that professional help is needed, insurance may pay for the visits. If you are not far from NYC, try Dr. Peter Green’s staff. Melinda Dennis at Beth Israel in Boston is good, she may perhaps consider a Skype session. Good Luck!!